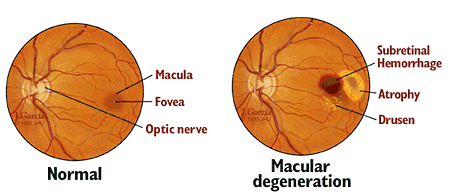
 An important component of any comprehensive eye examination is the retinal health assessment, which may be completed using either dilation or retinal imaging. During a retinal health check, an eye doctor evaluates the health of several key structures in the back of the eye that can change with age. The optic nerve, which sends signals to the brain, is assessed for signs of glaucoma. Evaluation of the arteries and veins by the eye doctor may indicate systemic disease such as high blood pressure, or diabetes. Another key structure of the posterior (back of) eye is the macula. The macula is responsible for the center part of our vision. Over time, the macula can deteriorate and lead to age-related macular degeneration, also known as “AMD.”
An important component of any comprehensive eye examination is the retinal health assessment, which may be completed using either dilation or retinal imaging. During a retinal health check, an eye doctor evaluates the health of several key structures in the back of the eye that can change with age. The optic nerve, which sends signals to the brain, is assessed for signs of glaucoma. Evaluation of the arteries and veins by the eye doctor may indicate systemic disease such as high blood pressure, or diabetes. Another key structure of the posterior (back of) eye is the macula. The macula is responsible for the center part of our vision. Over time, the macula can deteriorate and lead to age-related macular degeneration, also known as “AMD.”
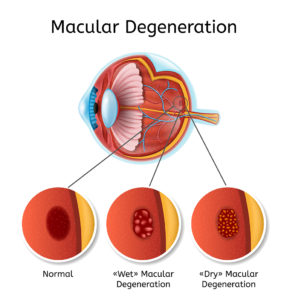
 AMD is the leading cause of severe, permanent vision loss in people over the age of 50 in the US. There are two types of macular degeneration, dry and wet. Dry macular degeneration is the most common form, ~80% of AMD patients. The macula begins to thin and accumulate lipid and protein deposits that form yellow clusters on the retina, known as drusen. This thinning and formation of drusen can disrupt the layer of photoreceptors in the retina and cause vision loss. Some of the symptoms associated with macular degeneration are blurry vision, straight lines appearing curved or wavy (metamorphopsia), dark or empty blind spots around the center of vision, or loss of central vision. There is no treatment for dry macular degeneration at this time; however, there are low vision devices or vision rehabilitation programs that help to manage the symptoms. Dry macular degeneration can progress to the second form of AMD, wet macular degeneration.
AMD is the leading cause of severe, permanent vision loss in people over the age of 50 in the US. There are two types of macular degeneration, dry and wet. Dry macular degeneration is the most common form, ~80% of AMD patients. The macula begins to thin and accumulate lipid and protein deposits that form yellow clusters on the retina, known as drusen. This thinning and formation of drusen can disrupt the layer of photoreceptors in the retina and cause vision loss. Some of the symptoms associated with macular degeneration are blurry vision, straight lines appearing curved or wavy (metamorphopsia), dark or empty blind spots around the center of vision, or loss of central vision. There is no treatment for dry macular degeneration at this time; however, there are low vision devices or vision rehabilitation programs that help to manage the symptoms. Dry macular degeneration can progress to the second form of AMD, wet macular degeneration.

Wet macular degeneration is usually more severe. Wet macular degeneration occurs when abnormal blood vessels begin to grow under the retina, causing swelling, bleeding and eventually scarring of the retina. Vision loss is more drastic with the wet form of AMD. The main form of treatment for wet macular degeneration consists of injections of anti-VEGF (vascular endothelial growth factor) which help decrease the abnormal leaky blood vessels that cause damage to the eye. Lasers can also be used in some circumstances.
A patient is at a higher risk of developing AMD if any of the following exist:
- Older than the age of 50
- Overweight
- Smoker
- Diagnosed with high blood pressure
- Diet high in saturated fats/high cholesterol
- Family history of AMD
- Caucasian
- Heart disease
The following lifestyle changes can help a patient reduce their risk of AMD, or the progression of AMD from dry to wet macular degeneration:
- Wear UV protection (Quality Sunglasses) when outside
- Quit tobacco use
- Eat a diet rich in antioxidants, vitamins and nutrients (leafy green vegetables)
- Maintain control of systemic disease
- Annual eye examinations – early and intermediate stages of macular degeneration may not present symptoms but can be diagnosed with a retinal exam. When it comes to AMD, early intervention and management of the condition is critical to minimizing the risk of disease progression and vision loss
MacuHealthPLUS+ vitamins are an effective dietary supplement that help to maintain healthy macular pigment and can reduce the risk of developing AMD. The supplements can also help those who have already been diagnosed with AMD by slowing the progression of the disease. With over a decade of scientific research, MacuHealthPLUS+ is recognized as the leading treatment protocol for those diagnosed with or at risk for Age-Related Macular Degeneration (AMD). Unlike other brands of eye vitamins, MacuHealth Plus provides all three forms of carotenoids that are present in the macular pigment. The supplement also provides a low dose of zinc, an essential mineral.
As a convenience for our Patients, we keep these vitamins in stock at Optometry at The Shops.
We look forward to seeing you at your next appointment!
Resources:
https://www.kcretina.com/blog/2020/01/23/aging-and-the-risk-of-203565https://www.aao.org/eye-health/diseases/amd-macular-degeneration
https://www.hopkinsmedicine.org/health/conditions-and-diseases/agerelated-macular-degeneration-amd